Blogs
 General Surgery
General SurgeryUnderstanding Chest Trauma: Causes, Effects, and Recovery
adminApr 19, 2024 Urology
UrologyComprehensive Guide to Prostate Surgery: Types and Considerations
adminApr 19, 2024 Infectious Diseases
Infectious DiseasesUnmasking Typhoid Fever: The Hidden Realities of a Deadly Disease
adminApr 19, 2024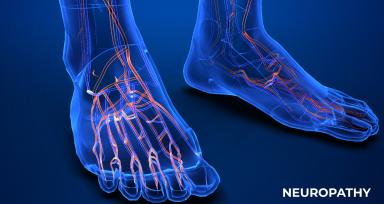 Neurology
NeurologyDiabetic Neuropathy
Dr. Kunal BahraniApr 19, 2024 Pulmonology
PulmonologyManaging Asthma: Identifying and Addressing Various Types of Asthma
adminApr 18, 2024 Orthopaedics
OrthopaedicsAll You Need to Know About Knee Replacement and Knee Resurfacing by Dr. Gagan Deep Gupta
Dr. Gagan Deep GuptaApr 18, 2024 Cardiac Sciences
Cardiac SciencesWhat is Arrhythmia: Understanding Types, Diagnosis, and Management
adminApr 17, 2024 Gastroenterology and Hepatobiliary Sciences
Gastroenterology and Hepatobiliary SciencesWhat is Non-Alcoholic Fatty Liver Disease (NAFLD)
adminApr 17, 2024 Infectious Diseases
Infectious DiseasesThe Role of Typhoid Vaccine as a Savior in Modern Times
adminApr 17, 2024 Oncology
OncologyThe Role of Genetics in Cancer Risk
Dr. Aakriti AggarwalApr 19, 2024