Ophthalmology
Corneal Imaging
Dr. Snehasis Basu Oct 16, 2019
Why corneal imaging
For the treatment of diseases or abnormalities arising out of corneal malfunctions, we need to assess the cornea. Though our aim is to understand how the cornea of a particular patient is working, we cannot photograph a corneal function. However, what we can do is to analyze in detail the structural intricacies of the cornea so we can indirectly infer from our gathered information as to how a particular cornea is working or will work in the future. This is the principle of corneal imaging. Needless to say, the more detailed the structural analysis, the better the accuracy of our diagnosis and as a result, the precision of treatment. This calls for data gathering and analysis. Application of digital analysis with superfast computers has helped us to achieve our goal which was not possible until a few decades earlier.Basic physiology
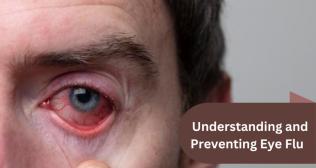
The eye is like a camera where the film is represented by the retina on the back surface of the eye, on to which the front lenses, represented by the cornea and the eye’s crystalline lens, focus light rays to form an image which we perceive as vision. About two-thirds of the light refraction of the eye takes place at the corneal surface and the rest at the lens. Hence, any alteration of the focusing power of the cornea or loss of its transparency will have a great impact on a person’s vision and result in various symptoms like a blurry image, a distorted image, a cloudy vision, and/or various discomforts like grittiness, eye ache, etc. When all parts of the cornea work in unison, we get a perfect image. If all the rays from the cornea are not focused to a point, the image precision suffers. It follows that if the analysis of the cornea is not done over a reasonable area of the cornea, it is likely to be faulty. While each individual point on the cornea is focusing an object perfectly, taken together they may not work in unison and this behavior may give rise to what is called an optical aberration.The cornea is like a watch glass. Its absolute clarity is maintained by the back surface of the cornea which constantly pumps out water from the cornea to prevent water-logging and thus prevents corneal cloudiness. Assessment of this back layer is very important in corneal diagnosis.
Different types of imaging
Corneal Topography
Corneal Topography assesses the uniformity of the front surface of the cornea where most part of light refraction takes place in the eye. Its predecessor is the conventional keratometry which has been used for the last 100 years or so. However, with keratometry, the information was restricted to a small apical cap on the cornea. The corneal topography, on the other hand, assesses the whole of the corneal front surface generating an immense amount of data and the processing of this huge data became possible only after the advent of advanced computer processors and RAM. Corneal Placido Topographers measure geometrical corneal slope values. These values are converted into curvature values e.g. axial (sagittal) curvature or instantaneous (tangential) curvature, to generate a corneal power map. The prototype is the Orbscan topographer (a Placido-based and slit-scan topographer).Corneal Tomography
Assessment of the corneal front surface only is not sufficient in various situations, because a significant amount of refraction takes place on the corneal back surface as well. So the back surface assessment can give a truer picture of corneal function. Also assessing the back surface correctly enables us to measure the corneal thickness precisely. As precision in corneal pachymetry, i.e. thickness measurement, became possible, the screening of patients for LASIK surgery and glaucoma diagnosis became easier. The tomographers, in contrast to the topographers, measure geometrical height (elevation) values. These values are converted into curvature values axial (sagittal) curvature or instantaneous (tangential) curvature, to assess corneal power distribution. The prototype is exemplified by Pentacam (Oculus Inc.). With the precise localization of the corneal back surface with the corneal tomographers, the diagnosis of keratoconus, a condition of corneal ectasis, became easier, as also the LASIK screening and the diagnosis of post-LASIK ectasia.Anterior Segment and Fourier-domain Optical Coherence Tomography (OCT)
At a reasonable working distance, the 5 ?m resolution of the Fourier-domain OCT device is much higher than that possible with corneal topography systems, where a maximum resolution achievable is between 50 ?m and 100 ?m (Orbscan II). Faster measurements of OCT also help in eliminating motion artifacts and consequently precision in diagnosis. Photographing the super-thin 100 ?m flaps of a femtosecond assisted LASIK became possible with the advent of the OCT. The precise imaging provided by the OCT helps in diagnosing and treating the various complication of the current version of corneal grafting, the Descemet Stripping Automated Endothelial Keratoplasty, or DSAEK. Examples are graft dislocation, primary graft failure, anterior chamber crowding, and papillary block. Corneal imaging with OCT also helps in the quantitative assessment of the anterior chamber angle by measuring with precision the various parameters e.g. the angle opening distance (AOD), the angle recess area (ARA), and the trabecular space area. OCT can also provide valuable information in assessing the depth required for phototherapeutic keratectomy (PTK) to remove visually significant stromal opacities, in diagnosing flap-related complications of LASIK like the Interface Fluid Syndrome, and in assessing the amount of corneal infiltrates in refractory microbial keratitis.The OCT is now comparable and in some situations, superior to the older method of Ultrasound Biomicroscopy (UBM).
Ultrasound Biomicroscopy (UBM)
In UBM a high-frequency ultrasound probe is used to image the reflected echoes from various eye structures. The exact configuration of the iris, ciliary body, and ciliary processes can be defined and their relation to the cornea assessed. At 10-50 ?m the resolution of UBM is less than that of OCT and has been largely superseded by the OCT. However, the UBM has value in cases of hemorrhage (as in ocular trauma) or in cases of dense corneal opacities, where the laser light of the OCT cannot penetrate tissues. White-to-white, sulcus-to-sulcus, and angle-width measurements are easily performed with UBM. These values can be quantified and compared after treatment. The main disadvantage of the UBM is that it requires a water bath as the coupling medium for the scan.Specular microscopy
This is another common method of corneal imaging. Specular microscopy is used to determine the cell density and the cell morphology of the corneal endothelium. Because cataract surgery causes some loss of endothelial cells, the risk of postoperative corneal decompensation is increased if preoperative endothelial cell counts are low. Abnormal endothelial cell morphology, including enlargement (polymegethism) and irregularity (pleomorphism), may limit the cornea’s ability to withstand stress. A specular microscope works on the principle of the specular reflex, which occurs at a regular, smooth-surfaced interface of two refractive indices with the light from the subject having an angle of incidence equal to the angle of reflection to the observer. All the presently available instruments utilize computer interfacing for image capture and endothelial cell morphology analysis. The instrument can be either of the contact types which touches the corea to flatten it and enlarge the generated specular reflex. The non-contact instruments utilize automatic image focusing technology. The specular reflex area of the latter is smaller than the contact types because of the curved corneal reflecting surface. Assessing the corneal endothelial surface in cases of prospective LASIK patients too, because contact lenses can cause transient and chronic endothelial cell morphology changes.Corneal Aberrometry
This assessment is often done using a machine called a wavefront aberrometer. By bouncing light off the retina and measuring the imperfections of the eye, the wavefront aberrometer creates a three-dimensional map of the cornea. This corneal map is then used for pre-operative screening to designing a customized ablation or tissue removal that addresses the patient’s unique aberrations, or imperfections. Customized ablation is used in both PRK and LASIK procedures. Some of the wavefront aberrometer in the market are OPD-Scan (Nidek Inc), KR1-W (Topcon Inc), and LADARWave (Alcon Inc).Confocal Microscopy
Analysis of each of the five layers of cornea can be done with the technic of confocal microscopy by simultaneously illuminating and imaging a single point of tissue by a scanning laser and thousands of points of tissue are then constructively joined to create the final confocal image. Some of the devices are NIDEK Confoscan, Heidelburg HRTII. Applications include the assessment of the endothelial cell layer, quantifying pathology of the subbasal nerve plexus in patients with neurotrophic keratopathy, and diabetic neuropathy involving the cornea, measuring the depth of structures, such as deposits, scars, or LASIK flaps as with the OCT. Confocal microscopy is a useful diagnostic means to help rapidly identify microorganisms in vivo, such as fungi or Acanthamoeba, so appropriate treatment can be initiated. This is akin to performing light microscopy on living tissue. This is particularly helpful because these organisms show scanty or no growth in ordinary culture media and hence a diagnostic confusion may arise unless confocal microscopy is used or a special culture technique is used.Future directions
Application of the swept-source technology (SS-OCT) with the advantage of increasing the depth penetration, and ultra high-resolution OCT (UHR-OCT) for a sub 5 ?m resolution will enable earlier and more precise diagnosis of corneal diseases.Categories
Clear allMeet the doctor

Dr. Snehasis Basu
SENIOR CONSULTANT OPHTHALMOLOGY | Fortis Anandapur
- Ophthalmology | Ophthalmology
-
31 Years
-
1000