Neurosurgical Emergencies At Home – When To Rush To A Hospital?
Even during the difficult times of Covid-19 infection, there is a chance of a Neurosurgical Emergency at home. During lockdown, it was noted that illnesses and hospital visits were reduced. This was partially true because the incidence of road accidents and other communicable diseases had reduced. Apart from that hypertension and stress were less when people were sitting at home and spending time with their families. Still, there is a chance that there is some acute problem related to the brain or spine that needs immediate attention. Telemedicine is an important medium through which consultation is possible without exposing to undue risk of Covid-19 infection. However, in certain cases immediate or urgent visit to the hospital is advisable.
We shall discuss them under various headings:
A. New brain or spine-related problem in a healthy person
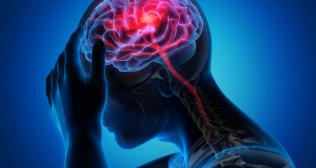
1. Sudden severe headache: this may be a symptom of a brain hemorrhage. This headache doesn’t get relieved with medication and may be associated with vomiting, seizure, weakness of limbs, or unconsciousness. The most common predisposing factor is raised blood pressure which leads to the rupture of a weak blood vessel. Angiography is required to find the cause and a large clot (hematoma) may need surgery. Immediate hospitalization is needed at a well-equipped center. Time should not be wasted in first-aid and the patient should shifted in your own vehicle or an ambulance.
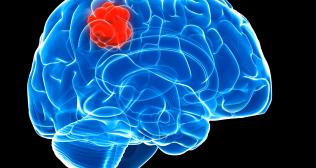
2. Chronic persistent headache: this may be due to migraine, tension headache, brain tumor, minor brain hemorrhage, or infection in the brain. In migraine, the headache is typically throbbing, on one side, associated with nausea or aura, and episodic. Usually, the patient is aware of his migraine and knows how to treat it. New onset migraine needs clinical evaluation and prophylactic treatment. Tension headache is usually in the evening due to stress and is relieved by pain-killers and sleep. Doctors may be consulted through telemedicine. Brain tumors may be associated with vomiting, vision or hearing loss, drowsiness, change in behavior, seizure, or weakness in limbs or face. Headache due to infection may have associated neck stiffness, fever, malaise, or drowsiness. Minor brain hemorrhage may be due to old head injury or slow continuous bleeding. All these require urgent consultation by a Neurosurgeon or Neuro-physician. MRI, CT scan, or angiography may be required to diagnose which is possible in a well-equipped hospital.
3. Seizure: anyone can suffer from a seizure (fit, epilepsy) for the first time at any age in life. It can be due to fever, brain tumor, brain hemorrhage, brain infection, or systemic illness. But in the majority of cases, no cause is found. Several investigations are needed to find the cause of seizure, especially blood sugar and serum electrolyte levels. A seizure episode may last for a few seconds to a few minutes. There may be a single episode or repeated episodes. Usually, it settles in 10-20 minutes and the person becomes normal. When someone throws a seizure, he should be made to lie down on the floor or bed with his body turned on the sides. Then we should loosen his clothes, avoid crowding, avoid giving water or food, prevent any injury, and wait for it to abort spontaneously. Seizure is self-limiting in 99% of cases. Once the person is normal (usually after 20-30 minutes), he can be taken to a hospital for consultation. In case there are repeated uncontrolled seizures (status epilepticus), an ambulance has to be called. In a patient who is a known case of seizure disorder may have recurrence when he misses the medication. He can consult through telemedicine and visit electively. Anti-epileptic nasal sprays can be prescribed by a doctor to abort the attack in patients with refractory disease. A medical consultation is necessary after any episode of seizure.
4. Sudden weakness in the face or limbs or one-half of the body, or loss of vision or speech: this can be due to stroke. Stroke is a medical emergency and can be cured by early intervention. If there is no headache, vomiting, or seizure, and only one-sided limb or facial weakness is noted then stroke is strongly suspected. Loss of vision, inability to speak, and imbalance while walking can also happen due to stroke. A stroke usually occurs in the elderly, but recently a lot of cases of ‘stroke in young’ have been noted. Predisposing factors are chronic illnesses like diabetes, hypertension, and cardiac disease. Patients should be immediately transferred to a hospital with a dedicated ‘stroke unit’ with facilities for mechanical thrombectomy in a Neuro-cathlab.
5. Sudden unconsciousness: this can be due to a massive stroke or large brain hemorrhage. Loss of consciousness can be due to reduced blood flow to the brain, which can be due to heart attack or visceral injury. It can be a sign of a seizure, raised pressure inside the brain, or sudden mental shock. The patient should be made to lie down comfortably, avoid crowding, loosen the clothes, turn on the sides, and try to wake him up by calling him or sprinkling water on his face. Simultaneously ambulance is arranged and the patient is shifted to a hospital. If the patient doesn’t recover in 20 minutes, then it may be something serious.
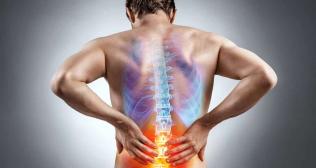
6. Severe back pain: sudden bending or lifting of heavy objects while doing household work is a common reason for sudden severe back pain in this period. Fall at home, ‘work from home’ in bad posture, past history of back pain, or some pathology in the back can be a cause for back pain. The immediate remedy for back pain is bed rest and tablets to reduce pain. Other options are hot or cold fomentation, local massage, analgesic gel application, or physiotherapy (microcurrent, short wave diathermy, ultrasonic, laser, or TENS). Usually, the pain reduces in 2-3 days, and no medical consultation is needed. In case the pain is not relieved and becomes chronic or is associated with limb weakness or numbness then urgent medical consultation is imperative. Rarely, pain may be due to minor fracture, acute disc prolapse, tumor, tuberculosis, or bony dislocation, which should not be neglected. A teleconsultation is a good option for back pain. Good posture, regular exercises, and a healthy diet are important to prevent back pain.
7. Weakness in limbs or neurological deficits: weakness or sensory loss in limbs or bladder or bowel involvement can indicate a nerve or spinal cord compression. This is a medical emergency and immediate hospitalization is required. Early intervention can reverse these deficits. Spinal cord compression may lead to weakness in limbs, difficulty in walking, tightness in limbs, difficulty in passing urine, constipation, sensory loss, and even difficulty in breathing. Nerve compression leads to pain, localized weakness, or loss of sensation. MRI of the spine is needed on an urgent basis and even surgery may be required.
B. A brain or spine problem in a patient who is already consulting a doctor
1. The patient wants to have a routine follow-up visit: teleconsultation is the best way to communicate with the doctor. Previous prescriptions should be shown to the doctor and fresh problems should be discussed. Old prescriptions are very helpful for the doctor to recognize you and your disease. Usually, no new investigations are required and minor changes in medication can be easily understood.
2. Problems have worsened or changed: In case the problem has worsened, video consultation can help to understand better. New investigations can be done and shared on e-mail or WhatsApp. The new medication is prescribed which can be followed judiciously. In case there is no relief then the doctor can be visited in person.
Categories
Clear allMeet the doctor

- Neurosurgery | Neurosurgery
-
20 Years
-
1500
 Available at 1 different locations
Available at 1 different locations









}}drupal-data/images/blog-lists.png)